

17075 Devonshire St., Suite 205 Northridge, CA 91325
16260 Ventura Blvd., Suite 600 Encino, CA 91436
555 Marin St., Suite 110 Thousand Oaks, CA 91360
Mon - Fri : 9:00 AM - 5:00 PM

Many patients with difficult asthma are undertreated or misdiagnosed. Our specialists evaluate for eosinophilic asthma, vocal cord dysfunction, and biologic eligibility.
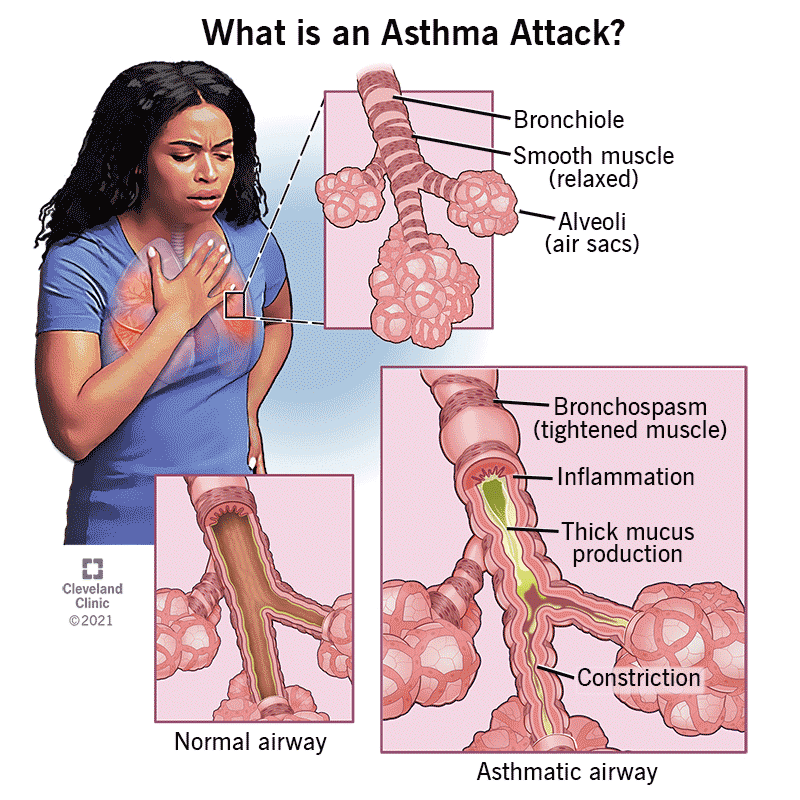
Asthma is a chronic inflammatory disease of the airways that causes recurring episodes of wheezing, breathlessness, chest tightness, and coughing — particularly at night or in the early morning. During an asthma episode, the airways become inflamed and narrowed, and mucus production increases, making it difficult to breathe. Between episodes, most people with well-controlled asthma feel normal. However, untreated or poorly controlled asthma can significantly limit daily activities and, in severe cases, lead to life-threatening exacerbations.
Asthma affects approximately 25 million Americans and is one of the most common chronic respiratory conditions seen by pulmonologists. Although it cannot be cured, asthma can be effectively managed in the vast majority of patients. When symptoms remain difficult to control despite standard therapy, further evaluation by a pulmonologist is essential to identify underlying causes, rule out mimicking conditions, and determine whether advanced treatments such as biologic medications are appropriate. Request an evaluation →
Asthma Care at PulmoCrit
Available at Northridge, Encino, and Thousand Oaks. Request an appointment →
Asthma results from a combination of genetic and environmental factors. A family history of asthma or other allergic conditions — such as eczema or hay fever — increases the risk. Common environmental triggers include allergens (dust mites, pet dander, mold, pollen), respiratory infections, exercise, cold air, tobacco smoke, air pollution, and occupational exposures such as chemical fumes or dust. In some individuals, aspirin or NSAIDs can trigger asthma, a pattern known as aspirin-exacerbated respiratory disease (AERD). Asthma can develop at any age, though it most commonly begins in childhood. Adults who develop asthma for the first time often have non-allergic forms of the disease, which can be more difficult to treat.
Not all asthma is the same. Understanding the underlying type helps guide treatment:
Asthma symptoms vary from person to person and may change over time. Common symptoms include:
Asthma cannot be diagnosed by symptoms alone — objective testing is essential. The cornerstone of diagnosis is spirometry, which measures airflow through the lungs before and after a bronchodilator (rescue inhaler). Reversible airflow obstruction — defined as a significant improvement in FEV₁ after bronchodilator administration — is characteristic of asthma. In patients with normal spirometry but suspected asthma, a methacholine challenge test can be used to assess airway hyperresponsiveness. Additional testing may include:
Asthma treatment is step-based — the intensity of therapy is matched to symptom severity and frequency. The primary goals are to achieve and maintain symptom control, prevent exacerbations, and preserve normal lung function with the minimum effective medication burden.
While many patients with mild asthma are managed by their primary care physician, a referral to a pulmonologist is appropriate when symptoms remain uncontrolled despite appropriate treatment, when the diagnosis is uncertain, when frequent exacerbations occur, when oral corticosteroids are needed repeatedly, or when biologic therapy is being considered. Pulmonologists also have access to advanced diagnostic testing — including bronchial challenge testing, FeNO, and comprehensive pulmonary function testing — that is not typically available in primary care settings.

Spirometry and comprehensive PFTs are the cornerstone of asthma diagnosis and monitoring. We perform in-house testing at all three locations.
Learn More
Cough-variant asthma is frequently missed. Our dedicated Cough Clinic uses a systematic protocol to identify asthma and other causes of chronic cough.
Learn More
A comprehensive pulmonary evaluation helps identify the cause of breathlessness, chronic cough, or exercise limitation — and ensures no diagnosis is missed.
Learn More