

17075 Devonshire St., Suite 205 Northridge, CA 91325
16260 Ventura Blvd., Suite 600 Encino, CA 91436
555 Marin St., Suite 110 Thousand Oaks, CA 91360
Mon - Fri : 9:00 AM - 5:00 PM

Ultrasound-guided thoracentesis performed in-office — no hospital admission required for most patients.
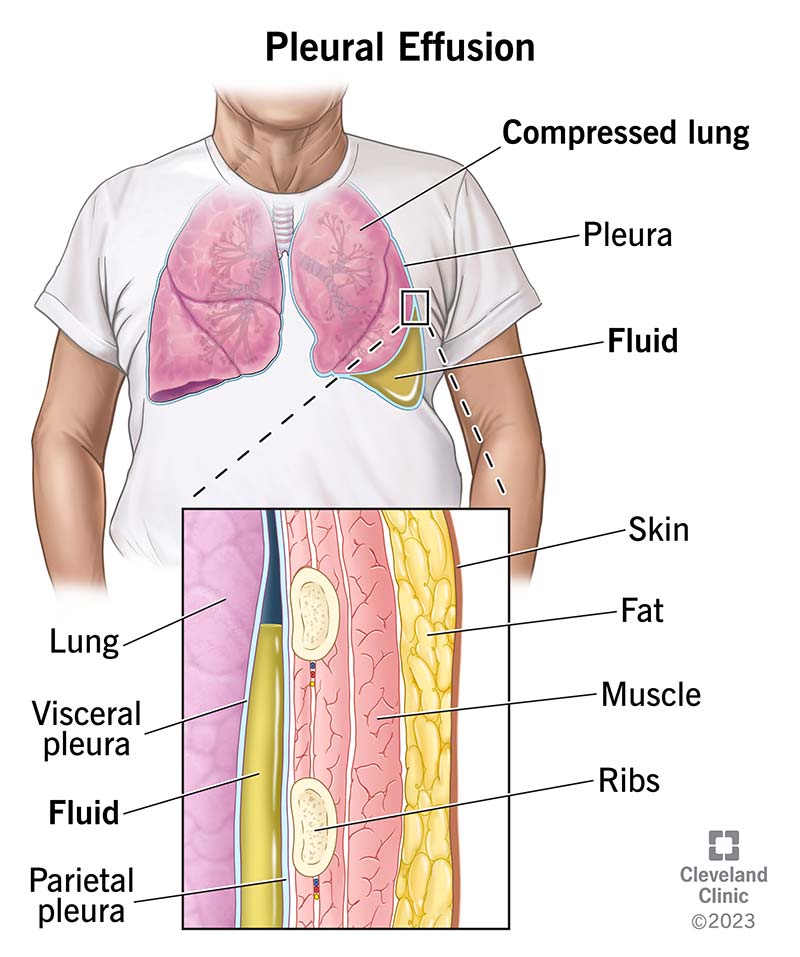
A pleural effusion occurs when excess fluid accumulates in the pleural space, the area between the lung tissue and the chest wall. Small amounts of fluid normally exist in this space to allow the lungs to move smoothly during breathing. However, when the balance between fluid production and reabsorption is disrupted, abnormal fluid accumulation can occur. Pleural effusions can develop from various underlying medical conditions and may range from asymptomatic to causing significant respiratory symptoms. Proper diagnosis and treatment of the underlying cause are essential for successful management and prevention of complications.
Pleural Disease Care at PulmoCrit
Available at Northridge, Encino, and Thousand Oaks. Request an appointment →
Pleural effusions can develop from numerous underlying conditions, broadly categorized as transudative or exudative:
Symptoms of pleural effusion vary depending on the size of the effusion and the underlying cause. Many small effusions are asymptomatic and discovered incidentally on imaging. Larger effusions typically cause shortness of breath, chest pain that worsens with breathing, dry cough, and reduced exercise tolerance. Diagnosis begins with clinical evaluation and imaging studies. Chest X-rays can detect moderate to large effusions, while ultrasound and CT imaging provide more detailed visualization. Pulmonary evaluation by our specialists includes assessment of your medical history and physical examination. To identify the underlying cause, thoracentesis (needle aspiration) is often performed to obtain pleural fluid samples for laboratory analysis.
Thoracentesis is a minimally invasive procedure in which a needle is inserted into the pleural space under ultrasound guidance to remove fluid samples for analysis. This procedure serves both diagnostic and therapeutic purposes. Diagnostically, the fluid is analyzed for characteristics such as protein content, cell counts, glucose, lactate dehydrogenase, and cultures to identify infections or malignancy. Therapeutically, removing excess fluid can provide immediate symptom relief and improve breathing. The procedure is generally safe and well-tolerated when performed by experienced pulmonary specialists, with minimal discomfort to the patient.
Treatment of pleural effusions focuses on addressing the underlying cause while managing symptoms. Depending on the diagnosis, treatment may include:
Following initial treatment, regular monitoring is important to assess response to therapy and detect complications. Our team at PulmoCrit Associates provides comprehensive follow-up care including repeat imaging, clinical assessments, and repeated thoracentesis if needed. For recurrent effusions, we work closely with you to optimize treatment of the underlying condition and prevent further fluid accumulation. Close collaboration with your primary care physician and specialists managing other conditions is essential for optimal outcomes.

A minimally invasive procedure to safely remove fluid from around the lungs for diagnosis and symptom relief.
Learn More
Comprehensive evaluation of pleural effusions and their underlying causes by board-certified pulmonary specialists.
Learn More
Advanced diagnostic testing to assess lung function and determine the impact of pleural effusions on your respiratory health.
Learn More