

17075 Devonshire St., Suite 205 Northridge, CA 91325
16260 Ventura Blvd., Suite 600 Encino, CA 91436
555 Marin St., Suite 110 Thousand Oaks, CA 91360
Mon - Fri : 9:00 AM - 5:00 PM

Airway clearance, culture-guided antibiotic therapy, and pulmonary rehab — a structured program built for bronchiectasis.
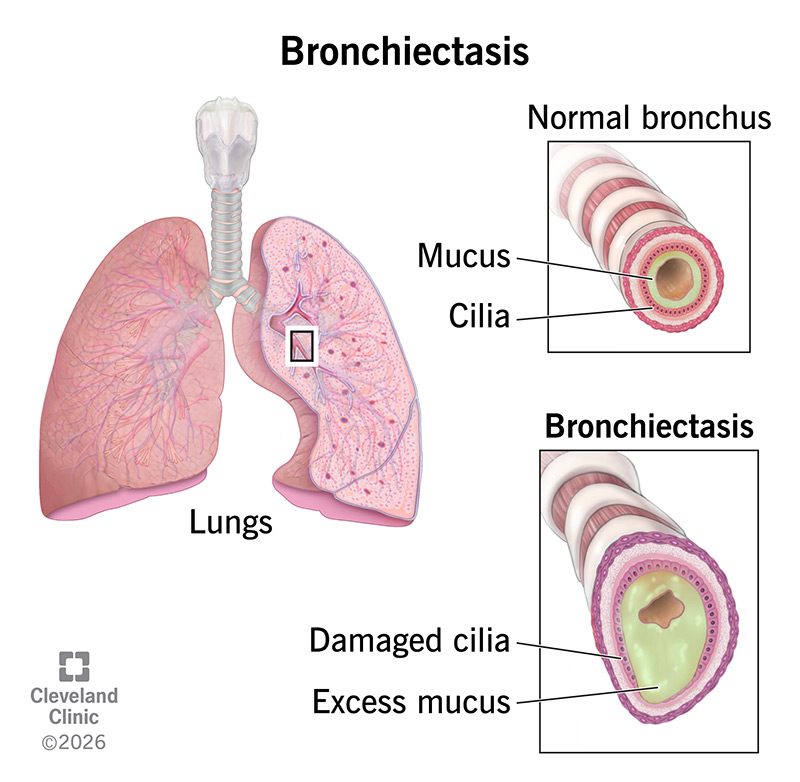
Bronchiectasis is a chronic lung condition characterized by permanent damage and abnormal widening of the airways (bronchi). This structural damage prevents the lungs from clearing mucus effectively, leading to recurrent respiratory infections, chronic cough, and progressive deterioration of lung function. Unlike asthma or COPD, which involve temporary narrowing of the airways, bronchiectasis involves irreversible structural changes to the bronchial tubes. The condition can range from mild to severe, depending on the extent of airway damage and the underlying cause. With proper management and treatment, many individuals with bronchiectasis can control symptoms and slow disease progression.
Bronchiectasis Management at PulmoCrit
Available at Northridge, Encino, and Thousand Oaks. Request an appointment →
Bronchiectasis can develop as a result of various underlying conditions and risk factors:
Common symptoms of bronchiectasis include chronic productive cough (often with large amounts of sputum), recurrent respiratory infections, shortness of breath, wheezing, and chest pain. Some individuals may cough up blood (hemoptysis). Diagnosis involves a combination of clinical evaluation and imaging studies. High-resolution CT scans of the chest are the gold standard for diagnosing bronchiectasis, showing the characteristic dilation of the airways. Pulmonary function testing helps assess the degree of airway obstruction and lung damage. Your physician may also order sputum cultures to identify specific bacterial infections and assess baseline lung function.
While bronchiectasis cannot be cured, comprehensive treatment can help control symptoms, prevent complications, and slow disease progression. Key components of management include:
A comprehensive pulmonary evaluation and rehabilitation program is an important part of bronchiectasis management. These programs typically include exercise training, breathing techniques, education about disease management, and psychosocial support. Regular exercise helps maintain physical fitness and improves exercise tolerance despite the chronic nature of the disease. Our specialists will work with you to develop a personalized management plan that addresses your specific symptoms and lifestyle needs.
Regular monitoring is essential to detect complications early and adjust treatment as needed. Complications of bronchiectasis can include severe infections, respiratory failure, hemoptysis, and the development of other respiratory conditions. Our team at PulmoCrit Associates provides comprehensive follow-up care to ensure optimal disease management and early intervention when complications arise.

Bronchoscopy allows direct visualization of the airways and can help assess airway damage and obtain samples for diagnosis.
Learn More
Testing to measure lung function and assess the degree of airway obstruction in bronchiectasis patients.
Learn More
Comprehensive rehabilitation programs to improve symptoms, exercise tolerance, and quality of life for bronchiectasis patients.
Learn More